Consumer-Centric Healthcare: Rising costs of healthcare means patients are more financially responsible for their healthcare costs than ever before. Desiring a more retail-like healthcare experience, patients are seeking providers who offer better opportunities to engage in their overall care. As a result, providers are focused on improving the patient experience and communicating with patients about their financial responsibility. Change Healthcare offers services and technologies that help providers improve the capture of patient financial data, increase collections, and improve the patient experience through better communication strategies at all points of service.
Financial Clearance Solutions
-Ahi QA: Helps providers improve the accuracy of patient registration data with real-time quality assurance and management tools.
-Ahi LobbyTM: Helps providers track patient flow, wait time, and patient service levels at registration.
-Clearance Patient Access Suite: Helps providers increase registration data accuracy, validate patients’ identity, complete insurance eligibility verification, secure preauthorization, estimate patients’ financial responsibility, accept point-of-service collections, and assist patients who are unable to pay as they consider financial assistance programs.
-Coverage InsightTM: Helps providers screen all patients, service types, and balance levels to identify missed or undisclosed reimbursement sources for patient accounts via advanced analytics.
Financial Clearance Services: Onsite and remote teams help hospitals improve collections by determining patient eligibility for insurance or other funding sources and assisting with enrollment. Our Eligibility & Enrollment Services and Financial Counseling help identify coverage and charity care and assists patients with setting up payment plans. Third Party Coverage helps identify reimbursement from motor vehicle accident and workers’ compensation claims.
Patient Experience Solutions
-Clearance Estimator: Helps hospitals and health systems create better patient estimates at or before the point of service to help increase collections and improve patient satisfaction.
-Clearance Price Transparency: Engages patients seeking price transparency with an interactive, easy-to-use portal.
-Patient Access Center Services: Patient access and call center services help hospitals and medical practices drive patient engagement, improve patient satisfaction, and optimize revenue.
Optimize Revenue and Reduce Risk:
Mid-cycle solutions from Change Healthcare help you optimize reimbursement by ensuring care is medically necessary and defensible, capturing all charges, supporting accurate claim coding, and maintaining coding compliance without adding pressure to your billing departments.
-Charge Capture Advisor: Combines artificial intelligence with an efficient workflow to predict missing charges prior to claim submission, automatically and proactively creating a more complete claim to help increase and accelerate revenue.
-InterQual®: An evidence-based clinical decision support solution to help ensure clinically appropriate medical utilization. The objective, comprehensive criteria enables defensible, consistent decision-making and an efficient way to proactively manage patient care to reduce length of stay, inappropriate admissions and readmissions, unneeded interventions and, in turn, denials.
-InterQual AutoReview™: A robotic process automation solution that pulls clinical data from your EHR to complete InterQual medical reviews automatically, instantly, and accurately, saving case management time. The automated reviews are enriched with real-time clinical data, increasing trust with your payers.
Revenue Integrity Services: These customer-centric services cover every specialty, meet virtually any volume need, and include care provided in both inpatient and outpatient facilities.
-Physician and Hospital Coding Services: Helps providers strengthen reimbursement and reduce risk by outsourcing or augmenting facility and professional fee-coding functions.
-Clinical Documentation Improvement Services: Helps improve the quality of clinical documentation and facilitates an accurate representation of healthcare services.
-Coding Quality and Audit Services: Helps mitigate risk by implementing quality review programs that verify accuracy and identify potential coding and compliance issues.
-Charge Capture Compliance Audit Services: Identifies missing charges to help optimize revenue and reduce the impact of negative cash flow.
Improve Revenue Performance
Our proven, end-to-end revenue cycle solutions can be customized to fit your organization’s specific needs. Leverage our 40+ years of physician and hospital billing and claims management experience to transform your revenue cycle and positively impact your organization’s financial health.
-Assurance Reimbursement Management™: Helps hospitals and health systems speed reimbursement and reduce costs by applying comprehensive business rules to claims, and by pairing automation and advanced workflow with meaningful reporting. This software solution helps to increase first-pass claim acceptance rates and utilizes artificial intelligence to identify claims at risk for denial so providers can address these claims before submission.
-Revenue Performance Advisor: Helps practices, labs, and other non-acute medical organizations get claims right the first time to avoid costly resubmissions and minimize denials. Revenue Performance Advisor software is integrated with practices’ existing workflows, enabling you to submit claims directly from your practice management or billing system.
Hospital and Physician Revenue Cycle Management Services
End-to-end revenue cycle management and medical billing services can provide as much—or as little— outsourcing help as you need. Our domain expertise in both physician and hospital billing and claims management, combined with decades of revenue cycle experience, can help your organization reduce operating costs, optimize cash flow and net patient revenue, and improve billing and collection efficiency.
-A/R Management: Revenue cycle and A/R management services for hospitals and health systems that want to become more operationally efficient and improve financial performance.
-Patient Responsibility Management: Self-pay patient collection services for hospitals and health systems that want to increase patient collections and shorten billing collection cycles.
-Business Office Outsourcing: A single-vendor resource for hospitals and health systems that want to drive incremental revenue improvement and lower cost-to-collect percentages.
-Denials and Appeals Management: Denials and appeals management services for hospitals that want to improve their clean-claims rate, better manage denied claims, and have expert assistance in handling appeals.
-Underpayment Audit and Recovery: Underpayment recovery services for hospitals that want to better manage denied claims and quickly correct healthcare underpayments.
Improve Consumer Payment Collection
-Build an Effective Payment Management Strategy
To increase patient collections, update your payment management strategy to reflect industry trends: Nearly one-third of all insured consumers are covered by high-deductible health plans (HDHPs)2, which means more of your patients are paying a larger portion of their healthcare expenses. With this increased financial responsibility comes a desire for more information and improved engagement. The shift to HDHPs parallels the rise in consumerism. As patients are taking an active role in purchasing and paying for healthcare services, we can assist this transition by providing more of a retail experience with convenient choices for both billing communications and payments, including online options.
-Communication and Payment Solutions Change Healthcare helps providers build an effective payment management approach encompassing three key strategies:
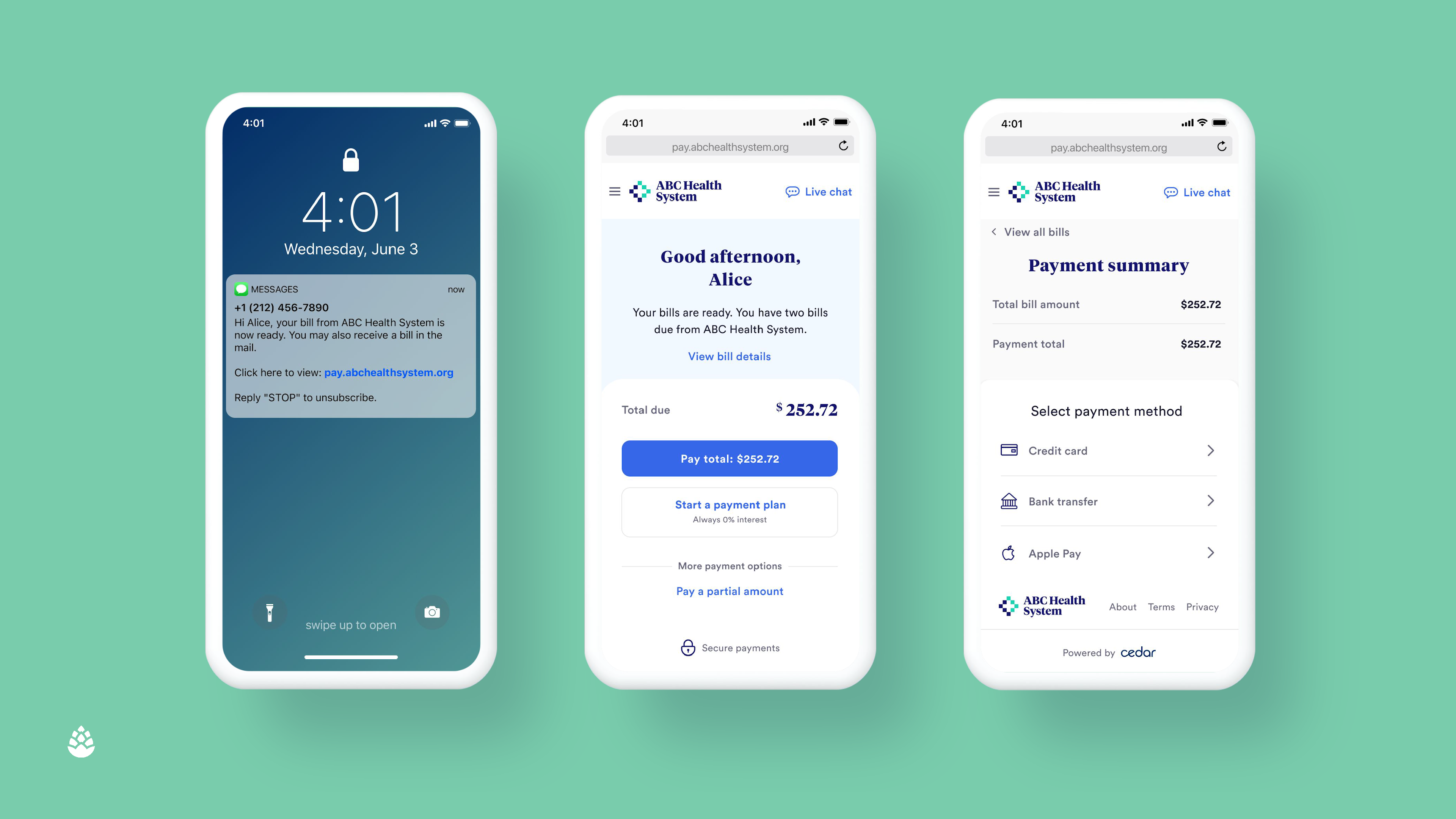
SmartPay™: Helps simplify the payment process with multiple, patient-friendly payment options to help drive collections. You can accept payments in-person, through the mail, online, and by phone.
-Patient Billing and Statements: Successful providers consider their print strategy as a way to send personalized communications designed to engage with consumers. We incorporate input from focus groups to maximize the effectiveness of your patient bills and statements, driving patient engagement, faster payments, patient satisfaction, and reduced print and mail costs.
-Payment Automation: Reduce the complexity and cost of processing both paper-based and electronic transactions by expediting and automating back-office payment processing and posting activities.
Acquire a Consumer- Centric Focus
• More than half of healthcare stakeholders surveyed consider patient engagement tools and services to be strategic necessities.3
• Accepting virtually all payment types during the patient visit (or via phone, online, or mail) can increase collections up to 224%.4
• Change Healthcare has industry-leading scale and capabilities, delivering 2.5 billion images per year, with 800 million documents mailed annually.5
To be competitive, your organization needs to understand the drivers of performance, the impact of quality on financial outcomes, and the benefits of potential efficiency gains. These insights can be obtained with a more comprehensive view of your patient, population, network, revenue cycle, and organizational health. We help you connect and transform disparate data points into actionable insights and help you benchmark with your peers, so you can make more informed decisions across your organization.
Our Financial Analytics Solutions Include:
-Acuity Revenue Cycle AnalyticsTM: Analyze historical revenue cycle trends within and across facilities, and drill down to identify root causes of issues and drive corrective action. We help providers analyze financial performance and operational results in minutes, without burdening IT resources.
-Pulse Revenue Cycle Benchmarking TM: We help hospitals and health systems analyze timely, equitable data from hospitals across the country and from relevant payers to help leaders establish benchmarks, compare performance support negotiations, and justify decisions with supporting data.
-Enterprise Business Insight: We help healthcare organizations develop custom solutions designed to centralize organizational data for easy access and reporting.
-Performance Analytics: A healthcare analytics solution for providers that want to leverage financial, clinical, and operational data to improve quality, reduce cost and risk, and diagnose current issues with interactive analytics. Provides financial and clinical stakeholders with a strategic understanding of financial risk in relation to care quality—in real time.
2“Employer Health Benefits, 2018 Annual Survey” Kaiser Family Foundation, October 2018
3“The 9th Annual Industry Pulse Survey” A national survey of leading health plans and other healthcare stakeholders
commissioned and conducted by the HealthCare Executive Group and Change Healthcare, 2019
4Internal Change Healthcare data; results are not guaranteed.